CE / CME
PrEP Made Practical: HIV Prevention in Mental Health Care Settings
Physician Assistants/Physician Associates: 0.75 AAPA Category 1 CME credit
Pharmacists: 0.75 contact hour (0.075 CEUs)
ABIM MOC: maximum of 0.75 Medical Knowledge MOC point
Physicians: maximum of 0.75 AMA PRA Category 1 Credit™
Nurse Practitioners/Nurses: 0.75 Nursing contact hour
Released: April 14, 2026
Expiration: April 13, 2027
Activity
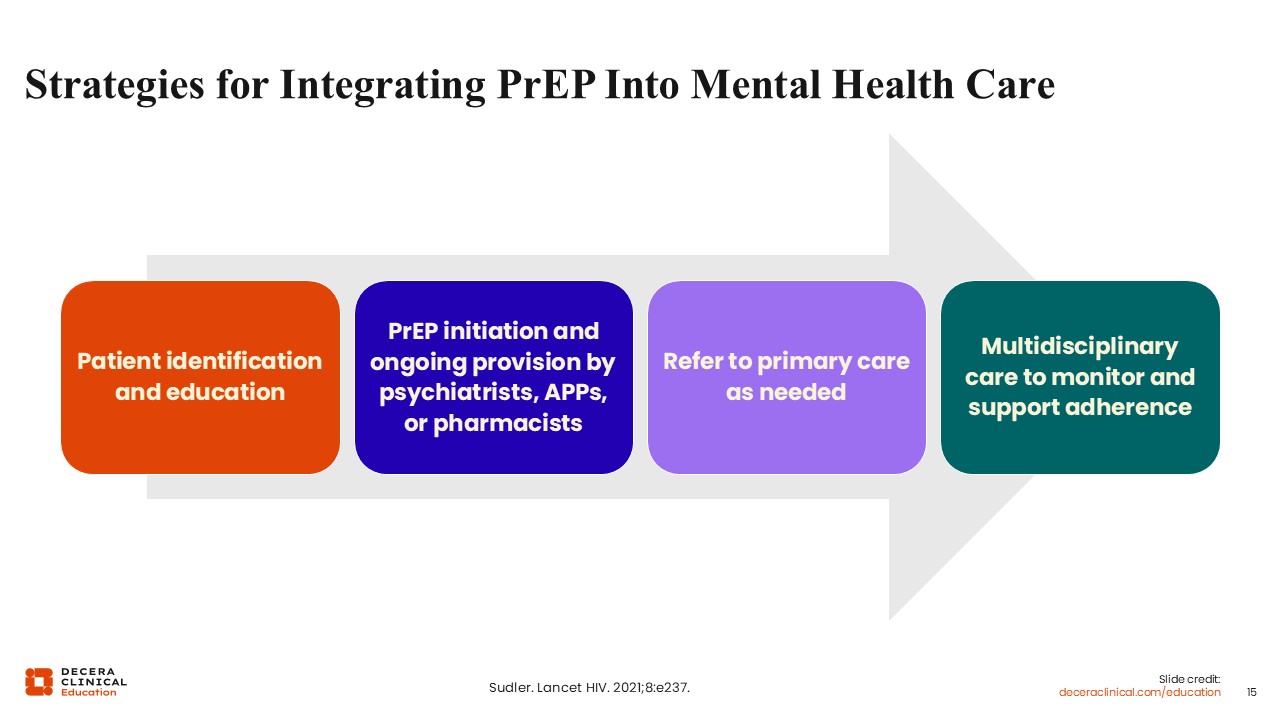
Strategies for Integrating PrEP Into Mental Health Care
Now that you are familiar with the basics of PrEP and how easy it can be, in this section, we’ll explore how you can integrate it into your mental health care practice.
Once you have identified people who could benefit from PrEP, I’ll show you how you can initiate and monitor within your psychiatric or mental health practice. If you cannot initiate medication, you can always refer people to primary care for consultation and PrEP provision, though that may increase the risk of loss to follow-up.6
If You Can Prescribe, You Can Help Prevent HIV!
If you practice in a mental health care setting and can prescribe treatment to your patients, then you should be aware of PrEP and coordinate access to it. Whether you are a psychiatrist, psychologist, an APP like a nurse practitioner or physician associate, or a pharmacist, depending on applicable state law, anybody with prescriptive authority can prescribe PrEP.
If you feel uncomfortable prescribing PrEP, you can partner with local psychologists, primary care, community organizations and clinics, and your state’s health department to facilitate access.
Roles for the Whole Mental Health Care Team
Regardless of ability to prescribe, everyone who practices in mental health care settings has a clear role in preventing HIV.
First, everyone should normalize PrEP by educating patients about it, raising awareness among colleagues, and reducing the stigma associated with it.
Second, patient education is an intervention. Repeating simple messages about PrEP over multiple visits can improve people’s readiness and follow-through.
Finally, because people with mental health conditions may see their mental health care professional more often than they see other HCPs, this provides a clear opportunity for us to use these touchpoints to keep PrEP on the agenda.6,22
Mental Health Care Nurses: High-Impact Touchpoints
Mental health care nurses play a particularly key role. They can help people understand PrEP and educate them about the importance of adherence.
I also think those in nursing who provide SUD or OUD treatment should be educated on HIV prevention strategies, including PrEP. That is because nurses can help reassure prescribing HCPs that PrEP is a critical component of harm reduction and whole-person care. They also can assist prescribing HCPs in initiating PrEP and monitoring people who are on PrEP.22,23
Nonprescribers in Mental Health Care
HCPs who do not have prescribing authority, such as psychologists, should link up with a psychiatrist to facilitate access to PrEP. This is especially helpful considering that many people with major depressive disorder or psychosis are involved in psychotherapy and psychiatric care with psychologists but see psychiatrists for their pharmacotherapy needs. It is a common model in mental health care for psychologists to manage the majority of patient care while the psychiatrists manage any pharmacotherapy.
Other therapists can operate similarly. That is why I believe all therapists should be educated on PrEP and should be able to talk with people about its benefits and risks. These HCPs can then encourage their patients to discuss further with their psychiatrist if interested in starting PrEP.6,22
Referrals: Partner Pathways if You Do Not Provide PrEP
Primary care can initiate and monitor PrEP, too. A persistent challenge with this, unfortunately, is that some primary care HCPs do not view HIV prevention as within the scope of their practice. Many feel this should be done by specialty care, yet most people without HIV are not being seen by HIV/STI specialists. Furthermore, no primary care HCP would be reticent to evaluate and treat gonorrhea or chlamydia in those who present with an infection, but they might feel like HIV PrEP is outside of their scope. Therefore, greater education is needed to help primary care providers understand that if they are treating STIs, then they also should be educating on and providing PrEP.
Same-Day PrEP Initiation: A Strategy to Improve Access
Same-day PrEP initiation is a strategy that many people have advocated for to improve access to PrEP.
Consider a person who presents to your clinic and indicates to you that they are at risk of acquiring HIV—say they have a partner with HIV who prefers condomless sex, or they share needles for injection drug use. You can test them for HIV and have them return at a later date to initiate PrEP, but this might increase their risk of acquiring HIV during that wait time.
Instead, you can ensure access to PrEP and increase retention between evaluation and same-day PrEP initiation. Furthermore, this strategy reduces office visits and travel time, making healthcare more convenient. And like treating other diseases and disorders, same-day PrEP initiation matches the standard of care for other therapies. For example, if someone presents with major depressive disorder, most mental health care professionals certainly would initiate any needed therapy during that first visit.
It is important to note that this strategy is not ideal for everyone. Some reasons not to consider same-day PrEP initiation include systemic barriers like cost, prior authorization, care fragmentation, and lack of staff, laboratory, or pharmacy services. Other person-specific considerations include those with prior kidney disease, possible acute HIV infection, or the inability to follow up if laboratory results return abnormal.24,25
In addition, some people pop in and out of care frequently, and others are not very connected to care. Therefore, same-day test and treat with PrEP is something that each HCP must think about among their patient population and with individuals as well.
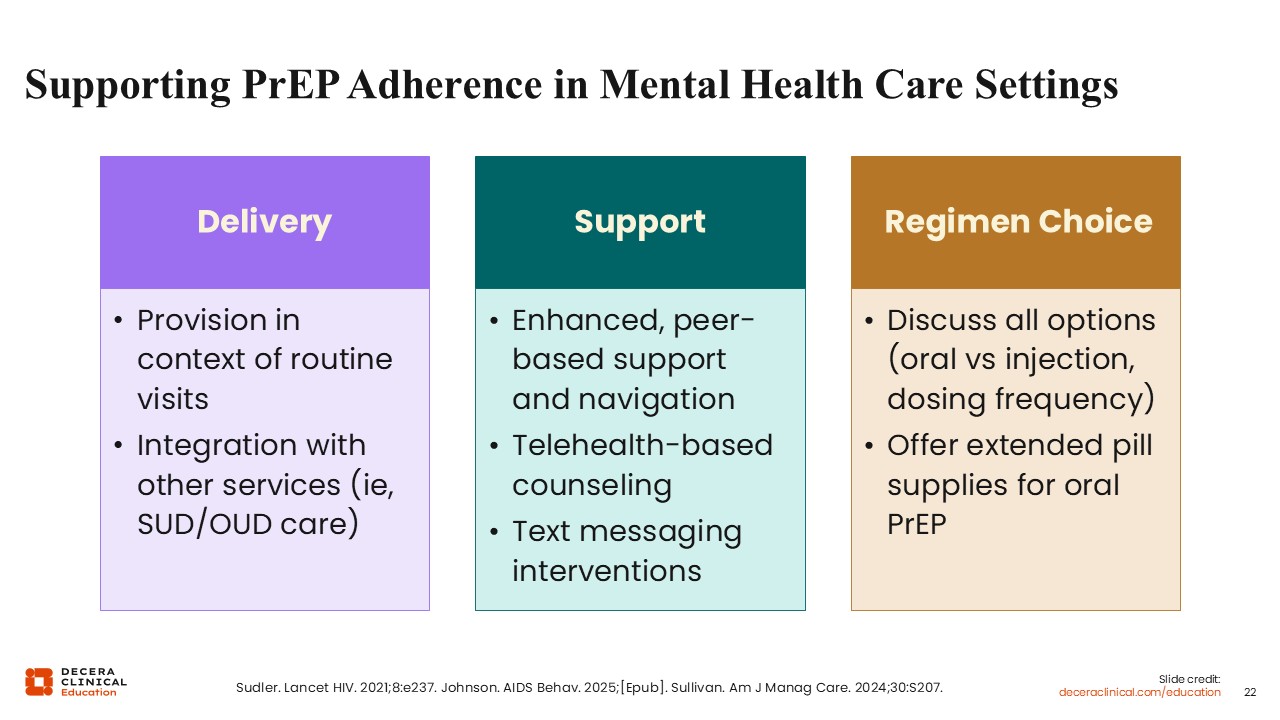
Supporting PrEP Adherence in Mental Health Care Settings
PrEP adherence can be encouraged in several ways. One is if it is delivered in integration with other services. Another important source of encouragement is peer-based support and navigation. Education and counseling may also help improve uptake and adherence.6,22,26
The NCCC PrEPline
For HCPs who are considering PrEP integration in their practice, the NCCC PrEPline is a good way to get a free tutorial on how to do so.
It is a teleconsultation service, operated by the University of California, San Francisco, that provides education and clinically supported guidance for PrEP decision-making.
Any US-based HCP can call the NCCC PrEPline. It is a valuable service because it offers individualized access to a multidisciplinary team of experts who stay current with the latest guidelines, literature, and best practices. They can tell you how to use PrEP at no cost.27,28
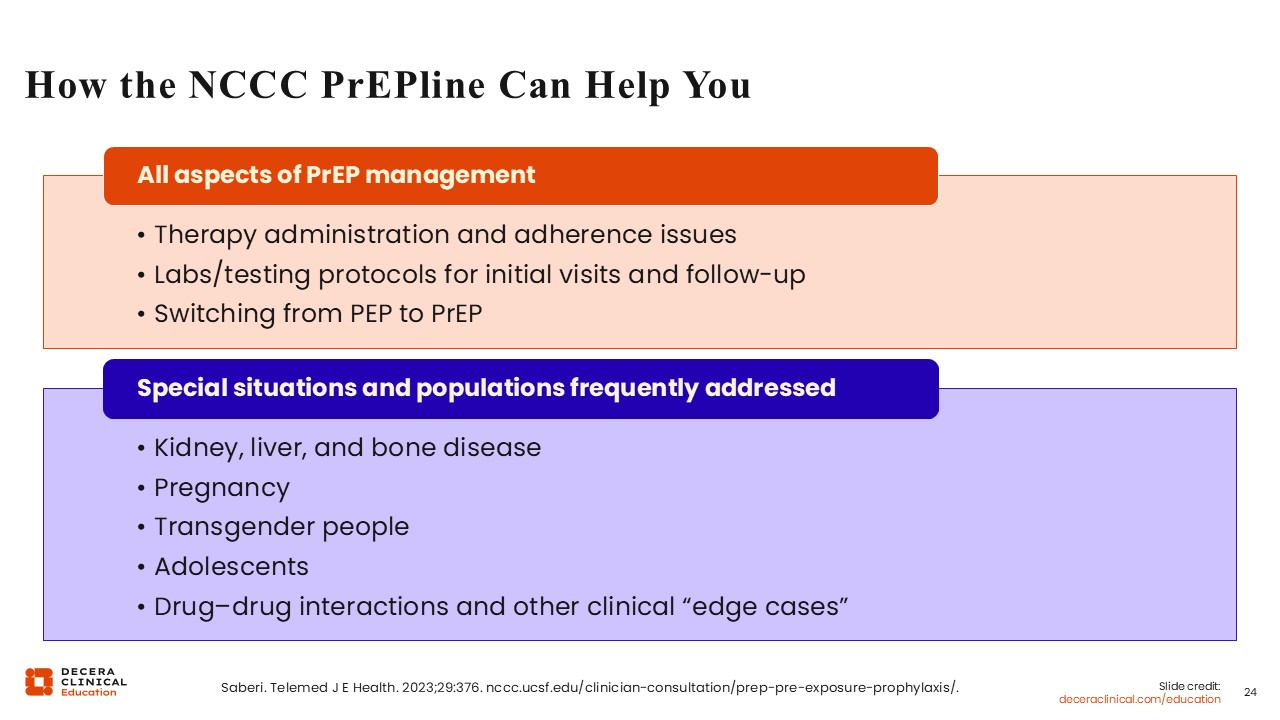
How the NCCC PrEPline Can Help You
This slide lists just some of the many ways that NCCC PrEPline consultants can help you with all aspects of PrEP management, including answering questions about administration, adherence issues, labs, and testing protocols for initial visits and follow-up, as well as switching from post-exposure prophylaxis to PrEP, which is such a good opportunity to improve prevention.29
The NCCS PrEPline can also help you with special situations and populations that you might not encounter as often.27,28
Accessing the NCCC PrEPline
The NCCC PrEPline is a great resource for those who are not yet sophisticated in PrEP and want to integrate it into their practice.
Questions and patient cases can be submitted via phone or through their website. Most are answered within 2 hours.28
Take-home Points
Those who are at risk of acquiring HIV are commonly seen in mental health care settings, and HIV prevention can be delivered in these spaces.
That’s why we, as mental health care professionals, can play a crucial role in stopping the HIV epidemic, given the risky behaviors or habits that some of our patients have. We cannot fully eradicate HIV without the buy-in and input from mental health care professionals.
On a more personal level, integrating PrEP into your mental health care practice will allow you to engage in a deeper way with your patients and allow them to have a better quality of life. PrEP not only prevents HIV acquisition, but it reassures patients that you are caring for them as a whole person and assessing all their needs.